On Wednesday, March 18, Candace Shaffer, AVP of Benefits & Payroll for Purdue University, co-presented with Elaine Murphy, SVP & General Manager for Rx Savings Solutions (RxSS), at the Conference Board’s 26th Annual Employee Health Care Conference in New York.
If you missed the session at Conference Board ‘26 or just need a solid recap, here are five key takeaways:
1.) Pharmacy benefits are increasingly difficult for members to navigate.
Rising GLP-1 utilization, specialty drug growth, tighter formularies, shifts to high-deductible plans, inconsistent pharmacy pricing, and mixed messages from discount cards and manufacturer programs create confusion and emotional stress for members trying to manage their costs.

Candace Shaffer, Purdue: I think our members have more choices today than even a year, certainly a couple of years, ago. So, it’s often up to them to try and make sense of everything. For expensive drugs, they might ask or hear about copay assistance through their prescriber or pharmacist or they see the advertisements. Maybe they qualify, maybe they don’t, right? For other medications, they can go online and find a coupon or use GoodRx. Or they might have direct-to-consumer or direct-from-manufacturer options. They don’t always know whether something is through the plan or the impact it has on their out-of-pocket cost or deductible.
2.) Transparency and simplicity are essential in helping members navigate prescription decisions.
Members face complex clinical, pricing, and benefit information, along with consumer marketing. Clear, understandable options and proactive support make it easier for them to manage their medications and make informed decisions.

Elaine Murphy, RxSS: Think of the experience we all went through in the travel industry before KAYAK® and Expedia®. You went to a retail travel agent who had all the information about flights and prices, hotel rates, etc., and were beholden to them to tell you what the cost of your vacation was going to be. Fast forward to 2026, we are all masters of navigating travel in our own way. Innovation changed an industry, and I believe we are at the beginning of that same experience with patient navigation in healthcare.
3. Employers and members need access to real-time affordability insights—not just tools.
Benefit leaders emphasize the importance of surfacing accurate, relevant affordability options at the exact moment they influence member decisions—across app experiences, prescribers, pharmacies, and throughout the full medication journey.

Candace Shaffer, Purdue: (Employers) can’t give personalized recommendations (to members) from a plan perspective, right? We can only provide the information. That just keeps everything complex, fragmented and just confusing for everybody.
Elaine Murphy, RxSS: You make a good point about your restrictions in abiding by fiduciary rules. The many rules and regulations in healthcare make it hard for all of us to navigate—not just from the consumer side, but the plan sponsor, providers, pharmacies… we each only have so much information (to work with).
4.) The future of pharmacy navigation is a more unified, low-friction ecosystem.
A more connected approach—bringing together affordability pathways, member engagement, prescriber and pharmacy touchpoints, and ongoing behavioral insights and ongoing behavioral insights—can help avoid member frustration, eliminate wasteful spending, and help members stay on the lowest-cost path as the market continues to evolve.

Elaine Murphy, RxSS: RxSS is in a good position to bring all of that together for the benefit of the patient so that they can make the decisions that are right for them. However, reliance on claims data can be limiting by how the industry is set up today. Insights are reactionary. We need them in real time to be actionable prior to that first fill, and we need them connected to more touchpoints.
One example we’re working on is pharmacy alerts [i], which will move us into the pharmacist workflow where we can actually populate an alert to help capture cost-saving opportunities on the first fill. This will be essential as we look at driving down cost in specialty.
5.) A member-centric pharmacy strategy has helped Purdue University’s health plan achieve strong engagement and meaningful pharmacy savings.
Over several years, Purdue has seen more than one-third of members engage with pharmacy decision support tools, contributing to more than $2M in savings—including $725K in 2025 alone[ii]. This reflects a sustained focus on helping members reduce out-of-pocket costs and optimize utilization.
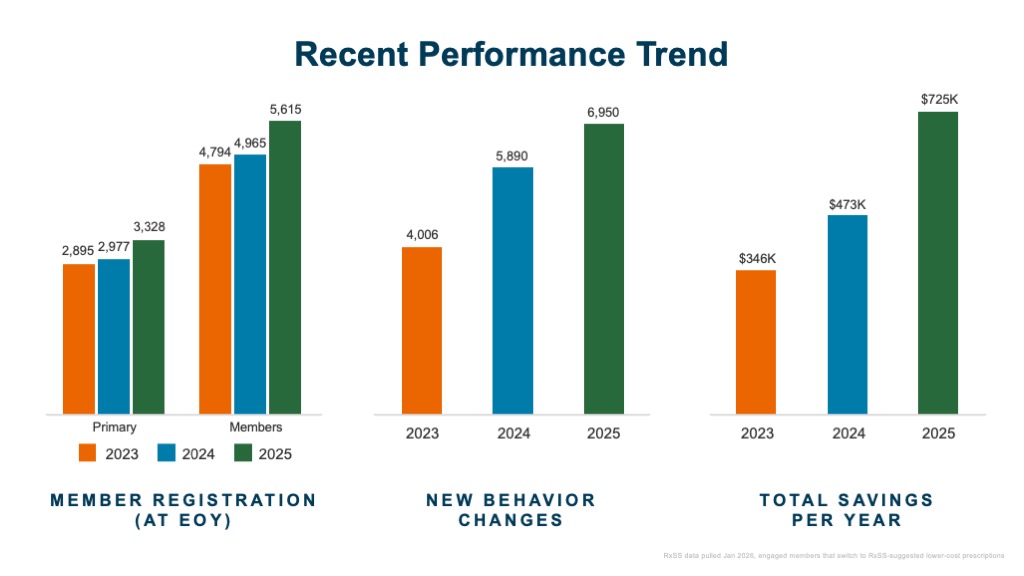
Registration – members that activated individual RxSS accounts
New behavior changes – members with unique switches to RxSS-suggested alternatives
Total savings – savings realized when engaged members changed to RxSS suggestions
Candace Shaffer, Purdue: For years, our goal has been to engage our members to stay on top of their prescription costs and empower them to take action. One of the difference makers for us has been the (RxSS) engagement tools, how they proactively notify about opportunities that matter to our members. They also get expert support when they want to enact those changes.
Elaine Murphy, RxSS: I think the data tells the story well, how Purdue’s engagement and savings have grown year over year. Behind that data is the partnership story. We see ourselves as true partners with your benefits teams. There is real value in that relationship. We have been able to work together to develop and deliver solutions that support your members and Purdue’s goals, whether in 2020 or 2030.
Candace Shaffer, Purdue: As benefit leaders, we need solutions now. But the question I think we will always ask is, how do we strike the balance between cost containment and member satisfaction? From our vantage point at Purdue, the right balance blends all these things—benefit design, cost sharing, education and empowerment—and above all, transparency and navigation support. Because things change from year to year, we need to evolve and innovate. It’s great to have a partner that can evolve with us.
[i] Any descriptions of future functionality reflect current product direction, are for informational purposes only and do not constitute a commitment to provide specific functionality. Timing and availability remain at McKesson’s, CoverMyMeds’ and Rx Savings Solutions’ discretion and are subject to change.
[ii] RxSS data pulled Jan. 2026, engaged members that switch to RxSS-suggested lower-cost prescriptions
